

-
Products
-
Solutions
- About Us
- Careers
- Exhibition Hall
-
Switch Language
Never give up; there is hope!
Arrhythmia led to cardiac arrest for 1-hour, cardiopulmonary resuscitation was ongoing for 1 hour, 4 times electrical defibrillation, 5 hours of life and death rescue, and finally brought the patient back from the brink or edge of death!
Mr. Yang, 64 years old, has been suffering from diabetes for more than 20 years and has multiple diseases such as coronary heart disease, hypertension, and (combined with) coronary heart disease, three-vessel disease. In the past year, repeated palpitations, chest tightness, shortness of breath, bilateral lower limbs edema, cannot lie down at night to rest, and long-term oral a variety of diuretic and cardiotonic drugs. At about 7:00 pm on July 3, he suddenly collapsed to the ground at home. He was in a daze, and his family immediately called 120.
When the pre-hospital emergency personnel arrived at the scene, they found that the patient had no vital signs, and his heartbeat, respiration, and pulse were undetectable!
Immediately, balloon-assisted ventilation, external chest compressions, and vital signs monitoring were performed. After being lifted into the ambulance, an intravenous channel was quickly established, and epinephrine was injected. The patient was rushed to the emergency department of Xixiang County People's Hospital.

The pre-hospital emergency doctor continued to perform external cardiac compressions on the patient while panting and reporting his condition to the receiving physician at the emergency department. The emergency medical staff on duty immediately placed the patient in the resuscitation room and took over from the prehospital emergency doctor continued to perform cardiopulmonary resuscitation on the patient. Although it was understood that the patient had three-vessel coronary artery disease and a history of ventricular fibrillation to syncope rescue a month ago, the probability of successful resuscitation is very low, but chest compressions are still being performed with all their strength. Finally, at the 23rd minute of compression, a miracle occurred; the patient recovered a weak voluntary heart rate!
Unfortunately, this weak voluntary heart rate only lasted for a short period of two minutes and then disappeared, but these short, "fleeting" two minutes gave the medical staff great confidence and motivation.
While the patient was undergoing continuous cardiopulmonary resuscitation, defibrillator defibrillation, endotracheal intubation, ventilator-assisted breathing, opening of venous access, bolus of epinephrine, amiodarone, blood drawn for testing...
The medical and nursing staff competed for time, each performed their own duties, and the resuscitation work was carried out in an orderly and intense manner. After nearly an hour of continuous chest compressions and a series of rescues, the patient finally recovered his voluntary heart rate after one hour of resuscitation but still had no spontaneous breathing and was in a comatose state, so the patient was sent to the ICU for further resuscitation treatment.
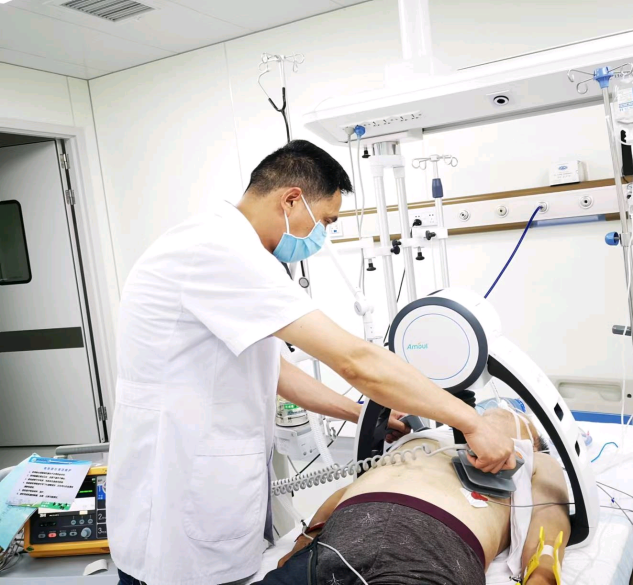
When the patient was first admitted to the ICU, his heart rate was maintained at 137 beats/min, his blood pressure was 272/235mmhg, and he was in a coma. Niu Dan and Cui Gang, the directors of the intensive care department, immediately organized the department staff to set up a resuscitation team, give ventilator-assisted breathing, analgesia, and sedation medication, and actively control blood pressure. After four hours of challenging resuscitation, the patient's blood pressure was stabilized at 145/95mmhg, and his heart rate was maintained at 100 beats/min.
After the patient's blood pressure and heart rate stabilized, the critical care medicine team used bedside B-ultrasound and hemodynamic monitoring equipment to accurately guide the patient's fluid intake and output, control the fluid intake and output per hour, and continued to follow the latest cardiopulmonary resuscitation guidelines and expert consensus. The patient underwent cerebral cardiopulmonary resuscitation, ice cap mild hypothermia treatment, and intracranial pressure monitoring guidance. At the same time, gastric tube and nasojejunal nutrition tube were given to maintain the normal physiological barrier of the intestinal tract, and intravenous fluid infusion was gradually reduced.
The medical and nursing staff kept constantly guarding, capturing every small change in the patient's vital signs, and the patient's condition was improving day by day. Finally, on the third day in the ICU, the patient's vital signs stabilized, and his state of consciousness changed from a coma to awake, which filled the family and medical staff with hope once again.
On the fifth day, the patient was successfully weaned off the ventilator, and the tracheal intubation was removed. The patient was encouraged to cough and sputum and was inspired to turn and pat his back and move his limbs to prevent deep vein thrombosis.
On the eighth day, the patient was fully conscious, his physical strength gradually recovered, and his appetite gradually increased. After a discussion with the family, he was transferred to the Cardiology Department for further treatment of the underlying diseases.
Take Better Care of Himself after Surviving
After continuing the cardiology department, such as cardiac diuresis and tube dilation, on July 15, the thirteenth day of admission, after the rest of his life, the patient, Mr. Yang, recovered and was discharged from the hospital. Talking about the gut-wrenching moment that day, Mr. Yang and his family expressed their gratitude to the medical staff of Xi Xiang County People's Hospital for their emergency and effective treatment, which saved his life from death. He gave a thumbs up, "This time, I escaped death by walking before the gate of hell. You gave me a second life. I will definitely care about my health in the future."
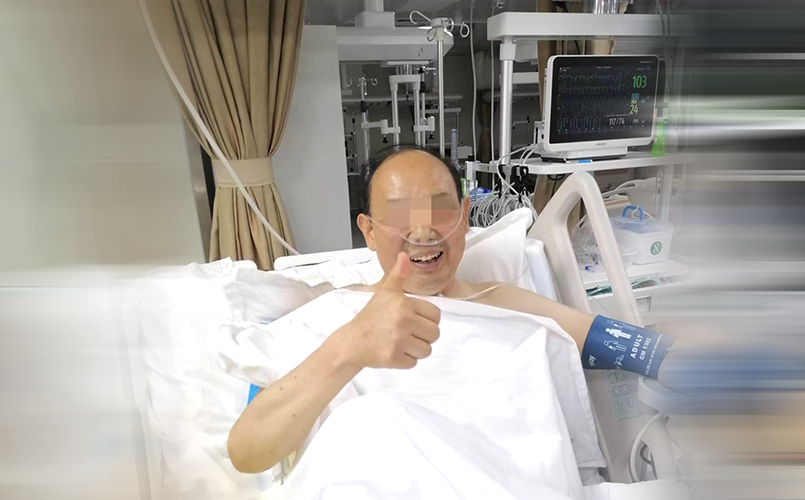
When he was discharged from the hospital, the cardiology staff advised Mr. Yang that he must pay attention to sustaining a healthy diet and preventing coronary heart disease. He also suggested quitting smoking, limiting alcohol, exercising moderately, keeping calm, avoiding mood swings, and developing an active lifestyle.
If a patient is in cardiac arrest and there is no sign of life after 30 minutes of resuscitation, they may not be able to return to life. But one hour after the cardiac arrest, after full resuscitation, the vital signs were restored, which is already a miracle in an emergency. However, no matter what difficulties they face, in the face of life, all medical personnel involved in resuscitation will do their best not to give up every patient, which is their eternal belief!
Miracle! Cardiac arrest for 1 hour! They successfully snatched a man from the hands of death! Xixiang County People's Hospital, 2022-07-21 17:31 Posted on Shaanxi. Available at: https://mp.weixin.qq.com/s/lYEERVyh2igJtW9fc1tXZA